No new serious adverse reactions were reported in the long-term extension study.

What is the most important information I should know about VIMIZIM?
Severe and life-threatening hypersensitivity reactions, including anaphylaxis, can occur during any VIMIZIM infusion, as early as 30 minutes from the start and up to 6 days after infusion, and as late into treatment as the 47th infusion. These reactions can occur in people receiving VIMIZIM for the first time or in people who have previously received VIMZIM without having an allergic reaction.
Your doctor will tell you about the symptoms of life-threatening hypersensitivity reactions, including anaphylaxis and when to seek immediate medical care. Typical signs of anaphylaxis include cough, rash, throat tightness, hives, flushing, changes in skin color, low blood pressure, shortness of breath, chest pain, and gastrointestinal symptoms such as nausea, abdominal pain, retching, and vomiting. If a severe allergic reaction (e.g., anaphylaxis) occurs during infusion, the infusion should be stopped immediately, and you should receive medical attention. Contact your doctor or get medical help right away if these symptoms occur after VIMIZIM infusions.
If you have a respiratory illness, you may be at risk for a sudden worsening of your condition, and you may require additional monitoring.
What else should I know about Vimizim?
VIMIZIM is a prescription medicine. Before treatment with VIMIZIM, it is important to discuss your medical history with your doctor. Tell your doctor if you are sick or taking any medication and if you are allergic to any medicines. Also tell your doctor if you are pregnant, planning to become pregnant, or are a nursing mother. Your doctor will decide if VIMIZIM is right for you. If you have questions or would like more information about VIMIZIM, contact your doctor.
You should receive medication such as antihistamines before VIMIZIM infusions to reduce the risk of reactions. If a reaction occurs, the infusion should be slowed or stopped and you may be given additional medication. If a severe allergic reaction (e.g., anaphylaxis) occurs during infusion, the infusion should be stopped immediately, and you should receive medical treatment.
If you have acute febrile or respiratory illness at the time of VIMIZIM infusion, you may be at higher risk of life-threatening complications from hypersensitivity reactions. If you use supplemental oxygen or continuous positive airway pressure (CPAP), you should have it available during your infusion in the event of a sudden reaction, or extreme drowsiness/sleep from antihistamines.
Spinal cord damage may occur due to the natural MPS IVA disease process. Signs of spinal cord injury include back pain, numbness and paralysis of limbs, and loss of bladder and bowel control. Contact your doctor immediately if you develop any of these symptoms.
What are the most common side effects of VIMIZIM?
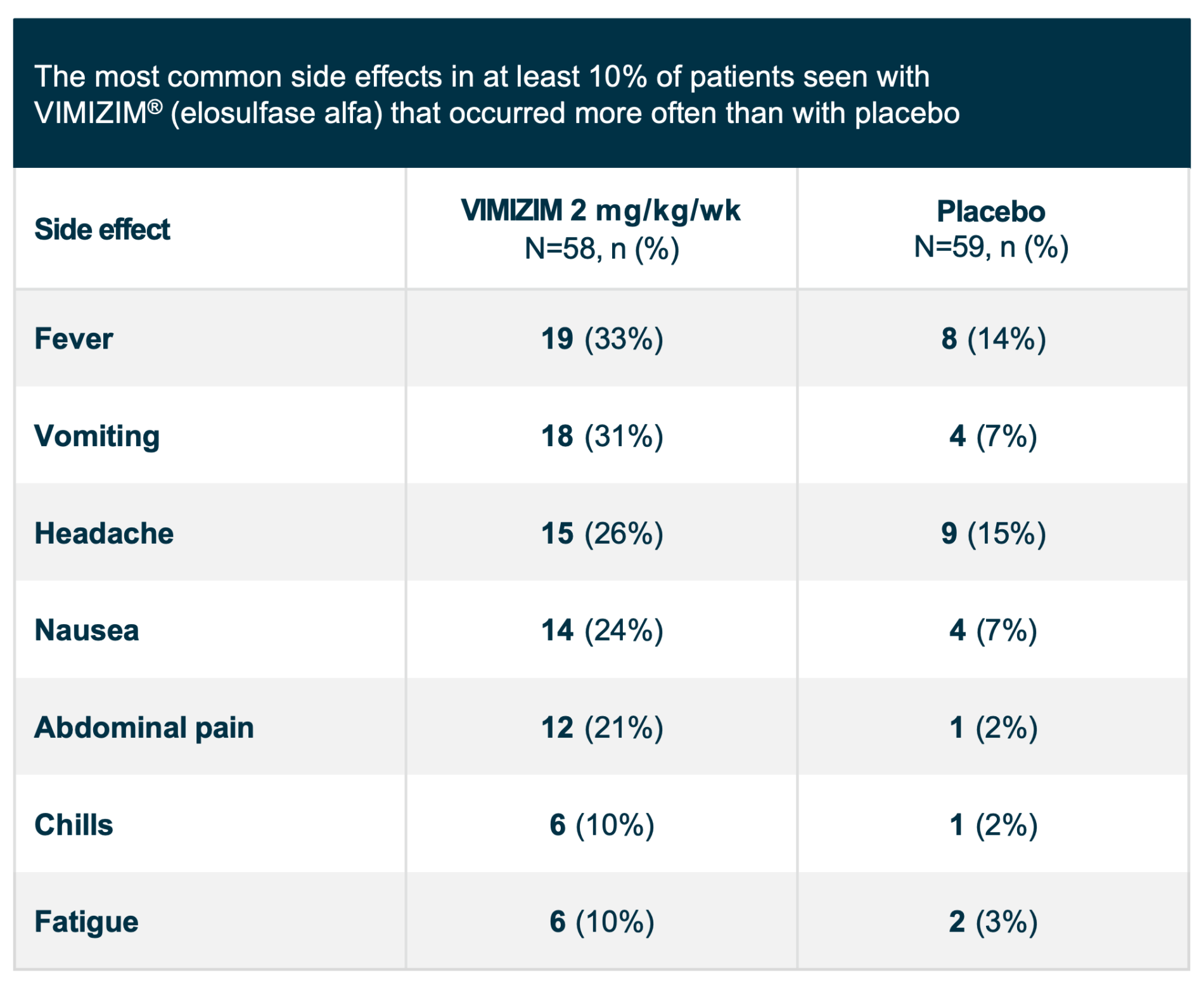
The most common side effects reported during VIMIZIM infusions included fever, vomiting, headache, nausea, abdominal pain, chills, and fatigue. These are not all the possible side effects with VIMIZIM. Talk to your doctor if you have any symptoms that bother you or that do not go away.
Call your doctor for medical advice about side effects. You may report side effects to BioMarin at 1-866-906-6100 and the FDA by visiting www.fda.gov/medwatch or calling 1-800-FDA-1088.
Please see full Prescribing Information, with important warning for risk of anaphylaxis.
VIMIZIM® (elosulfase alfa) is indicated for patients with mucopolysaccharidosis type IVA (MPS IVA; Morquio A syndrome).